Track your nutrition and health goals
Grade 3 Fatty Liver: Symptoms, Risks, Recovery Time & Treatment
By Dr. Sumedha Verma | Medically Reviewed | Updated April 2025
Grade 3 fatty liver is the most severe form of fatty liver disease.
At this stage, more than two-thirds of liver cells are filled with fat, and the risk of serious complications such as liver inflammation, fibrosis, and eventually cirrhosis becomes significantly higher.
This guide explains what Grade 3 means, what symptoms to watch for, how serious it is, and crucially, whether recovery is still possible.
| Important: Grade 3 fatty liver is serious but does not automatically mean liver failure. With specialist medical care and consistent lifestyle changes, the condition can be stabilised and, in many cases, improved. However, this stage requires immediate professional attention, not just dietary tweaks. |
|---|
What Is Grade 3 Fatty Liver?
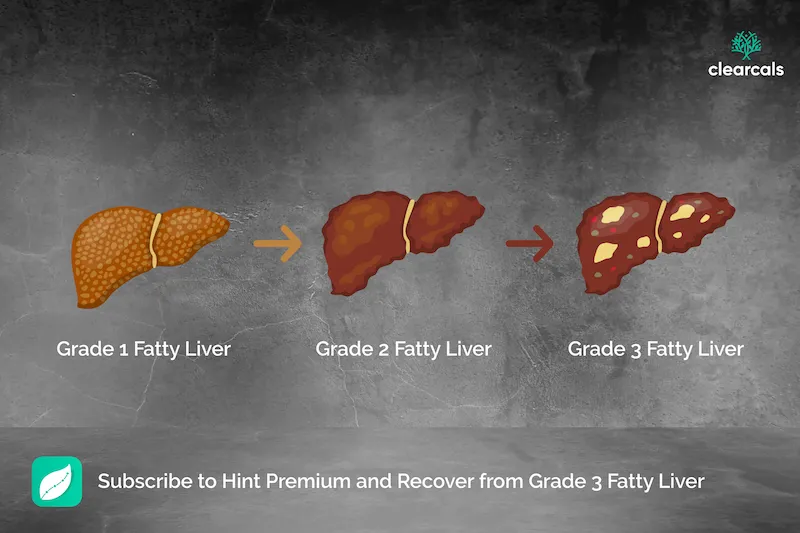
Fatty liver disease (NAFLD) is graded on a scale of 1 to 3 based on the percentage of liver cells (hepatocytes) affected by fat accumulation:
| Grade | Fat in Liver Cells | Severity |
|---|---|---|
| Grade 1 (Mild) | 5% to 33% | Low, often symptom-free |
| Grade 2 (Moderate) | 33% to 66% | Medium, liver under stress |
| Grade 3 (Severe) | More than 66% | High, specialist care required |
At Grade 3, the liver is under significant stress. The sheer volume of fat can trigger inflammation (a condition called NASH, non-alcoholic steatohepatitis). Without treatment, this inflammation can lead to fibrosis (scarring) and eventually cirrhosis or liver failure. The liver is also typically visibly enlarged (hepatomegaly) at this stage.
Compared to Grade 1 and Grade 2 fatty liver, Grade 3 fatty liver requires more intensive medical management alongside lifestyle changes. Self-management alone is not sufficient.
Symptoms of Grade 3 Fatty Liver
Unlike Grade 1, where most people have no symptoms, Grade 3 fatty liver often produces noticeable signs. However, symptoms can still be vague and easily mistaken for other conditions.
Common Symptoms
- Persistent fatigue and weakness that does not improve with rest
- Pain or a dull, persistent ache in the upper right abdomen (below the ribs)
- Abdominal swelling or a feeling of fullness, even when not eating much
- Nausea and reduced appetite
- Unintentional weight loss
- Elevated liver enzymes (ALT, AST) detected on blood tests
Warning Signs That May Indicate Progression to NASH or Fibrosis
- Jaundice: yellowing of the skin or whites of the eyes
- Dark-coloured urine or pale stools
- Severe abdominal pain or sudden swelling of the abdomen (ascites)
- Confusion or difficulty concentrating (a sign of hepatic encephalopathy in advanced cases)
- Spider-like blood vessels visible on skin (spider angiomas)
- Swelling in the legs and ankles
| If you experience jaundice, severe abdominal pain, confusion, or sudden leg swelling, please seek urgent medical attention. These may indicate progression beyond fatty liver to cirrhosis or acute liver stress. |
|---|
Skin and External Signs
Some people with advanced fatty liver develop visible skin signs, including darkening of the skin around the neck and armpits (acanthosis nigricans), which is more related to insulin resistance than the liver condition itself.
Others may notice extreme fatigue affecting their daily functioning, or subtle yellowing that they first notice in photographs.
Is Grade 3 Fatty Liver Dangerous?
Yes, Grade 3 fatty liver is a serious medical condition that requires prompt attention. However, 'dangerous' does not mean 'irreversible'. The key risks at Grade 3 include:
- Progression to NASH: Up to 20% of people with Grade 3 NAFLD develop non-alcoholic steatohepatitis, where inflammation actively damages liver cells
- Liver fibrosis: Prolonged inflammation causes scar tissue to form, stiffening the liver
- Cirrhosis: Advanced fibrosis can lead to cirrhosis, which significantly impairs liver function and is difficult to reverse
- Liver cancer (hepatocellular carcinoma): Though uncommon at the fatty liver stage, cirrhosis from NAFLD increases this risk
- Cardiovascular risk: NAFLD, particularly at Grade 3, is closely associated with increased risk of heart attack and stroke
The danger at Grade 3 is not the fat itself but what happens next if the condition is ignored: inflammation, fibrosis, and organ dysfunction. This is why specialist care (hepatologist or gastroenterologist) is strongly recommended at this stage.
Causes of Grade 3 Fatty Liver
Grade 3 fatty liver rarely develops overnight. It typically results from years of unmanaged risk factors, including:
- Severe obesity (BMI above 35), particularly central or abdominal obesity
- Type 2 diabetes with poor blood sugar control over many years
- Very high triglycerides (hypertriglyceridemia)
- Metabolic syndrome (a combination of high blood pressure, high blood sugar, excess abdominal fat, and abnormal cholesterol levels)
- Hypothyroidism (undiagnosed or poorly managed)
- Heavy alcohol consumption (alcoholic fatty liver disease)
- Certain medications: long-term steroids, methotrexate, tamoxifen, amiodarone
- Rare genetic conditions affecting lipid metabolism
How Is Grade 3 Fatty Liver Diagnosed?
Diagnosis typically involves a combination of imaging and blood tests:
- Abdominal ultrasound: identifies severe fat infiltration and liver enlargement; a Grade 3 liver appears very bright (echogenic) on ultrasound
- CT scan or MRI: provides detailed fat quantification and assesses the extent of liver involvement
- FibroScan (transient elastography): measures liver stiffness to check for early fibrosis
- Liver function tests: markedly elevated ALT, AST, GGT, and sometimes bilirubin
- Liver biopsy: occasionally recommended at Grade 3 to confirm NASH and assess the degree of fibrosis; invasive but definitive
- Your doctor may also refer you for an endoscopy if portal hypertension is suspected.
Grade 3 Fatty Liver Treatment
Grade 3 fatty liver requires a multi-pronged treatment approach under medical supervision. There is no single medication that reverses Grade 3 NAFLD, but the following interventions work together:
1. Medically Supervised Weight Loss
A 10% or greater reduction in body weight is associated with significant improvement, even in Grade 3. However, crash dieting or very rapid weight loss (more than 1.5 kg per week) can paradoxically worsen liver inflammation. A structured, medically supervised programme is recommended.
2. Strict Dietary Changes
At Grade 3, dietary discipline must be more rigorous than at earlier stages:
- Eliminate sugar, alcohol, and all refined carbohydrates
- Follow a Mediterranean-style diet or a low-glycaemic Indian diet
- Significantly reduce total calorie intake under a dietitian's guidance
- Ensure adequate protein intake to protect muscle mass during weight loss
- Refer to our Indian Fatty Liver Diet Chart for specific meal plans, with the understanding that Grade 3 may require a more calorie-restricted version.
3. Structured Exercise Programme
At Grade 3, start with low-impact aerobic exercise (walking, swimming) and gradually build up. Exercise reduces liver fat independently of weight loss. Aim for at least 200 minutes per week of moderate activity under medical supervision.
4. Medication Management
While no drug is specifically approved for NAFLD, your doctor may prescribe:
- Vitamin E (in non-diabetic NASH patients): has been shown to reduce liver inflammation
- GLP-1 receptor agonists (e.g., semaglutide): newer class of diabetes drugs showing promise for liver fat reduction
- Pioglitazone (in diabetic patients): improves insulin sensitivity and reduces liver inflammation
- Ursodeoxycholic acid (Udiliv): supports liver function and bile flow
- Statins: for cardiovascular risk management alongside liver disease
Always follow your hepatologist's prescription. Do not self-medicate with liver supplements or herbal remedies without medical guidance.
5. Regular Monitoring
Grade 3 patients require:
- Liver function tests every 3 months
- Ultrasound or FibroScan every 6 months
- Endoscopy is recommended if cirrhosis is suspected, to check for varices
- Annual HbA1c, lipid profile, and full metabolic panel
6. Bariatric Surgery (in Selected Cases)
For patients with severe obesity (BMI above 40, or above 35 with diabetes) where other interventions have failed, bariatric surgery can dramatically reduce liver fat and reverse even Grade 3 NAFLD. This is assessed on a case-by-case basis by a specialist team.
Grade 3 Fatty Liver Recovery Time: What to Expect
Recovery from Grade 3 fatty liver is possible, but takes significantly longer than earlier grades. Here is a realistic timeline:
| Timeframe | What Typically Happens | What to Monitor |
|---|---|---|
| 1 to 3 months | Liver enzymes begin to normalise with dietary changes | LFTs every 4 to 6 weeks |
| 3 to 6 months | Reduction in liver fat visible on ultrasound; weight loss progress | Repeat ultrasound, weight tracking |
| 6 to 12 months | Significant reduction in fat grade from 3 to 2 possible | FibroScan to check the fibrosis level |
| 12 to 24 months | Grade 3 can improve to Grade 1 or normal in motivated patients | Full metabolic panel, liver biopsy if needed |
| Can Grade 3 Fatty Liver Be Reversed? Yes, in many cases. Studies show that even Grade 3 NAFLD can regress significantly with aggressive but sustainable lifestyle changes and medical management. However, if fibrosis has already developed, it may only partially resolve. This is why early and consistent action is critical. |
|---|
Managing Grade 3 Fatty Liver with Hint Premium
Grade 3 fatty liver recovery is a long journey that requires sustained effort over 12 to 24 months. Hint Premium can support you throughout with:
- Personalised calorie and macro targets based on your health profile
- Specialist-designed Indian meal plans for Grade 3 liver management
- Weekly check-ins and progress tracking
- Medication and appointment reminders
- Access to certified dietitians for ongoing nutritional support
Download Hint from the App Store or Google Play. For Grade 3, we strongly recommend Hint Premium and coordination with your hepatologist.
Frequently Asked Questions
Can Grade 3 fatty liver be cured?
Fully cured in the sense of returning to a completely normal liver is possible, especially if fibrosis has not yet developed. With consistent treatment over 1 to 2 years, Grade 3 can improve to Grade 1 or even resolve. Once fibrosis develops, some scarring may be permanent, but liver function can still significantly improve.
Is Grade 3 fatty liver the same as cirrhosis?
No. Grade 3 fatty liver means severe fat accumulation, but not necessarily scarring or cirrhosis. However, it significantly increases the risk of progressing to cirrhosis if untreated. Cirrhosis is diagnosed separately, usually by FibroScan or biopsy.
What is the recovery time for Grade 3 fatty liver?
Most people see measurable improvement within 6 to 12 months with consistent lifestyle changes and medical management. Full regression from Grade 3 to Grade 1 or normal typically takes 12 to 24 months. Individual timelines vary depending on metabolic factors, adherence, and whether fibrosis is present.
Can I manage Grade 3 fatty liver with diet alone?
Diet and exercise are essential components, but Grade 3 usually requires medical supervision and often medication. Do not attempt to manage Grade 3 without consulting a hepatologist or gastroenterologist.
What foods are strictly off-limits at Grade 3?
Alcohol is an absolute contraindication. Beyond that, all added sugars, refined carbohydrates, fried foods, processed meats, and full-fat dairy should be eliminated or severely restricted. See our Indian Fatty Liver Diet Chart for what to eat instead.
Disclaimer: This article is for informational and educational purposes only and does not constitute medical advice. Always consult your doctor, gastroenterologist, or hepatologist for diagnosis and treatment guidance specific to your health condition.
About the Author
Dr. Sumedha Verma is a Consultant Physician at Clearcals with extensive experience in clinical medicine and healthcare services.
She has significant expertise in managing chronic conditions such as diabetes, thyroid disorders, PCOS, infertility, and other gynecological health concerns.
Known for her patient-centered approach, Dr. Verma focuses on improving patient compliance and helping individuals achieve better health outcomes through personalized medical guidance and long-term care.
🔗 Connect with Dr. Sumedha on LinkedIn